eBusiness Weekly

Dr.John Chamunorwa Mangwiro
M.D.MMED{Med}UZ.Consultant Specialist Physician ,Consultant Specialist Diabetologist
Diabetes is a global issue, affecting hundreds of millions of people worldwide. Many people describe diabetes as being a pandemic. There are several types of diabetes, in this issue we will discuss type 1, but first the Zimbabwean issue in brief.
The Zimbabwean situation
By Mutsa P. Gumbie ,Usha Gowda,John Chamunorwa Mangwiro and Andre Renzaho
Objective
Diabetes appears to be a growing problem in the African region. This study aims to estimate the prevalence of diabetes in Zimbabwe by collating and analysing previously published data.
Methods
Systematic review and meta-analysis of data reporting prevalence of diabetes in Zimbabwe was conducted based on the random effects model. We searched for studies published between January 1960 and December 2013 using MEDLINE, EMBASE and Scopus and University of Zimbabwe electronic publication libraries.
In the meta-analysis, sub-groups were created for studies conducted before 1980 and after 1980, to understand the potential effect of independence on prevalence.
Results
Seven studies were included in the meta-analysis with a total of 29 514 study participants. The overall pooled prevalence of diabetes before 1980 was 0,44 percent (95 percent CI 0,0–1,9 percent), after 1980 the pooled prevalence was 5,7 percent (95 percent CI 3,3-8,6 percent).
Conclusions
This study showed that the prevalence of diabetes in Zimbabwe has increased significantly over the past three decades. This poses serious challenges to the provision of care and prevention of disabling co-morbidities in an already disadvantaged healthcare setting.{1}
Type 1 diabetes
Name: Type 1 diabetes was formerly known as “juvenile diabetes” and “insulin-dependent diabetes.” These terms are inaccurate and obsolete. We know that it’s not just “juveniles” who get Type 1 diabetes — adults get Type 1, too, and many people who have Type 2 diabetes must take insulin. So, Type 1 diabetes is the correct term.
Type 1 diabetes mellitus (DM) is a multisystem disease with both biochemical and anatomic/structural consequences. It is a chronic disease of carbohydrate, fat, and protein metabolism caused by the lack of insulin, which results from the marked and progressive inability of the pancreas to secrete insulin because of autoimmune destruction of the beta cells.
Type 1 DM can occur at any age. It is most common in juveniles but can also develop in adults, especially in those in their late 30s and early 40s.
Unlike people with type 2 DM, those with type 1 DM usually are not obese and usually present initially with diabetic ketoacidosis (DKA). The distinguishing characteristic of a patient with type 1 DM is that if his or her insulin is withdrawn, ketosis and eventually ketoacidosis develop. Therefore, these patients are dependent on exogenous insulin.
Signs and symptoms
The classic symptoms of type 1 diabetes are as follows:
Polyuria
Polydipsia
Polyphagia
Unexplained weight loss
Other symptoms may include fatigue, nausea, and blurred vision.
The onset of symptomatic disease may be sudden. It is not unusual for patients with type 1 diabetes to present with diabetic ketoacidosis (DKA).
Diagnosis
Diagnostic criteria by the American Diabetes Association (ADA) include the following :
A fasting plasma glucose (FPG) level ≥126 mg/dL (7.0 mmol/L), or
A 2-hour plasma glucose level ≥200 mg/dL (11.1 mmol/L) during a 75-g oral glucose tolerance test (OGTT), or
A random plasma glucose ≥200 mg/dL (11.1 mmol/L) in a patient with classic symptoms of hyperglycemia or hyperglycemic crisis
Lab studies
A fingerstick glucose test is appropriate for virtually all patients with diabetes. All fingerstick capillary glucose levels must be confirmed in serum or plasma to make the diagnosis. All other laboratory studies should be selected or omitted on the basis of the individual clinical situation.
An international expert committee appointed by the ADA, the European Association for the Study of Diabetes, and the International Diabetes Association recommended the HbA1c assay for diagnosing type 1 diabetes only when the condition is suspected but the classic symptoms are absent.
Screening
Screening for type 1 diabetes in asymptomatic low-risk individuals is not recommended. However, in patients at high risk (eg, those who have first-degree relatives with type 1 diabetes), it may be appropriate to perform annual screening for anti-islet antibodies before the age of 10 years, along with 1 additional screening during adolescence.
Management
Glycemic control
The ADA recommends using patient age as one consideration in the establishment of glycemic goals, with different targets for preprandial, bedtime/overnight, and hemoglobin A1c (HbA1c) levels in patients aged 0-6, 6-12, and 13-19 years. Benefits of tight glycemic control include not only continued reductions in the rates of microvascular complications but also significant differences in cardiovascular events and overall mortality.
Self-monitoring
Optimal diabetic control requires frequent self-monitoring of blood glucose levels, which allows rational adjustments in insulin doses. All patients with type 1 diabetes should learn how to self-monitor and record their blood glucose levels with home analysers and adjust their insulin doses accordingly.
Real-time continuous monitoring of glucose — using continuous glucose monitors (CGMs)—can help patients improve glycemic control. CGMs contain subcutaneous sensors that measure interstitial glucose levels every 1-5 minutes, providing alarms when glucose levels are too high or too low or are rapidly rising or falling.
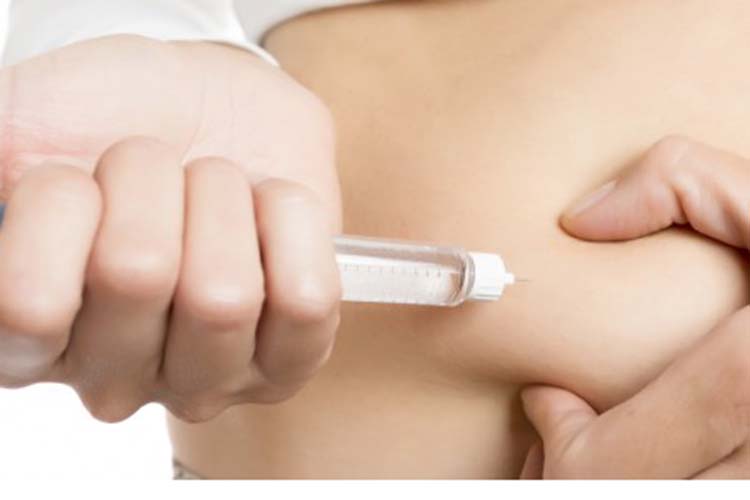
Insulin therapy
Patients with type 1 diabetes require lifelong insulin therapy. Most require 2 or more injections of insulin daily, with doses adjusted on the basis of self-monitoring of blood glucose levels. Insulin replacement is accomplished by giving a basal insulin and a preprandial (premeal) insulin.
The basal insulin is either long-acting (glargine or detemir) or intermediate-acting (NPH). The preprandial insulin is either rapid-acting (lispro, aspart, insulin inhaled, or glulisine) or short-acting (regular).
Common insulin regimens include the following:
Split or mixed: NPH with rapid-acting (eg, lispro, aspart, or glulisine) or regular insulin before breakfast and supper.
Split or mixed variant: NPH with rapid-acting or regular insulin before breakfast, rapid-acting or regular insulin before supper, and NPH before bedtime (the idea is to reduce fasting hypoglycemia by giving the NPH later in the evening).
Multiple daily injections (MDI): A long-acting insulin (eg, glargine or detemir) once a day in the morning or evening (or twice a day in about 20 percent of patients) and a rapid-acting insulin before meals or snacks (with the dose adjusted according to the carbohydrate intake and the blood glucose level).
Continuous subcutaneous insulin infusion (CSII): Rapid-acting insulin infused continuously 24 hours a day through an insulin pump at 1 or more basal rates, with additional boluses given before each meal and correction doses administered if blood glucose levels exceed target levels
Diet and activity
All patients on insulin should have a comprehensive diet plan, created with the help of a professional dietitian, that includes the following:
A daily caloric intake prescription.
Recommendations for amounts of dietary carbohydrate, fat, and protein.
Instructions on how to divide calories between meals and snacks
Exercise is also an important aspect of diabetes management. Patients should be encouraged to exercise regularly.{2}
References
- Prevalence of diabetes in Zimbabwe: A systematic review with meta-analysis, January 2015, Mutsa P. Gumbie ,Usha Gowda,John Chamunorwa Mangwiro and Andre Renzaho
- Type 1 Diabetes MellitusUpdated: Apr 21, 2017 Author: Romesh Khardori, MD, PhD, FACP; Chief Editor: George T Griffing, MD.



